• Chronic pelvic pain affects approximately 1/3 of all women and accounts for 15% of gynecology appointments
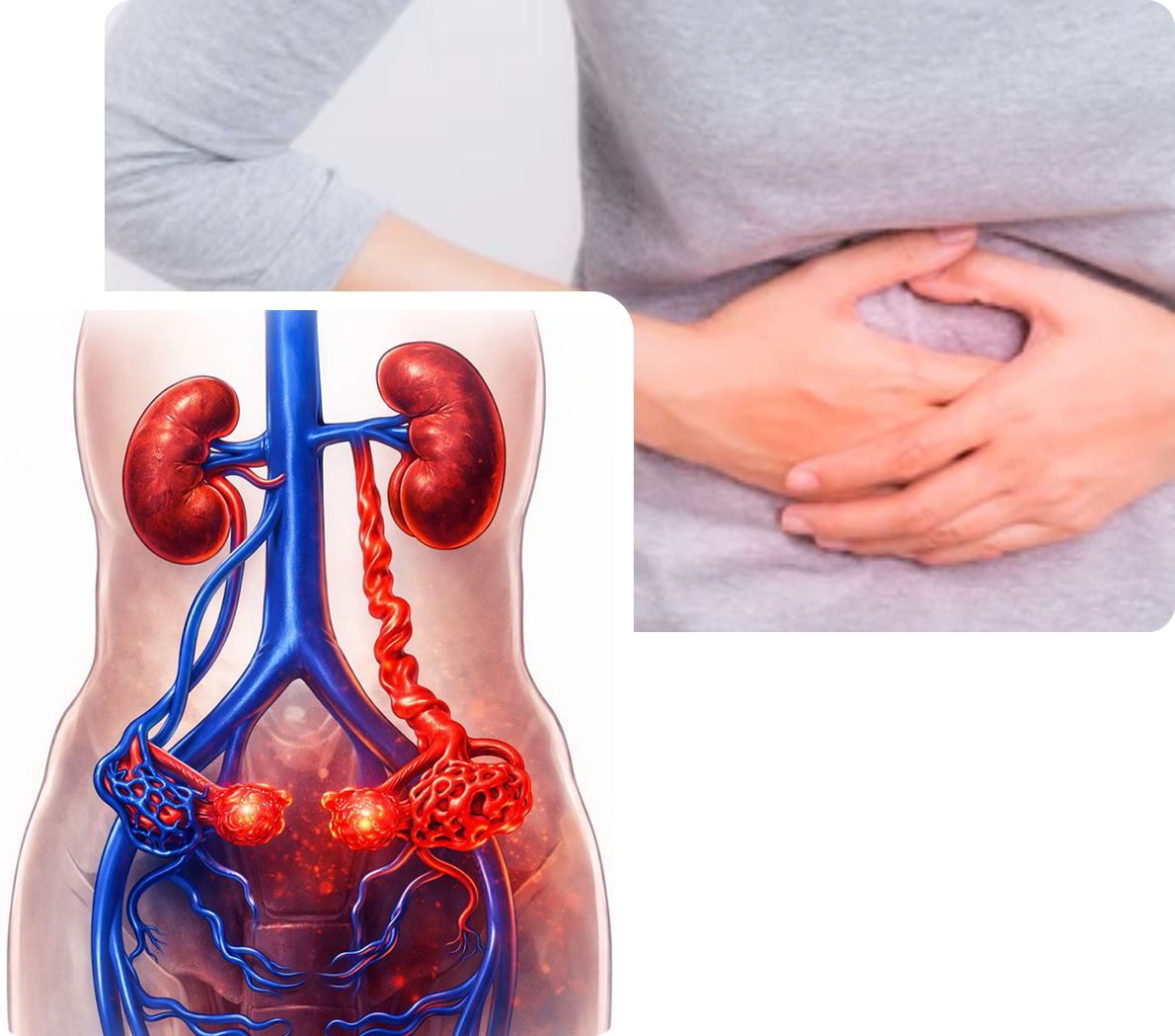
• PCS occurs as a result of damage to valves of the ovarian veins, allowing blood to flow backwards and pool in the pelvis
• Imaging findings of PCS are enlarged ovary veins and resulting varicose veins in the pelvis
• Up to half of all women evaluated for chronic pelvic pain are found to have varicose veins in the pelvis
• PCS is under diagnosed and likely effects about 10% of women
• Symptoms include lower abdominal and pelvic pain and pressure, worsened with standing, menses, exercise, pregnancy, or intercourse
• Hip or leg pain may occur and bulging varicose veins can develop on the vulva and upper legs
• Medical management with hormones that suppress ovarian function. Often provides only temporary relief
•Surgery: Ligation (suturing) of the ovarian vein is the most invasive option and may not completely treat the abnormal veins.
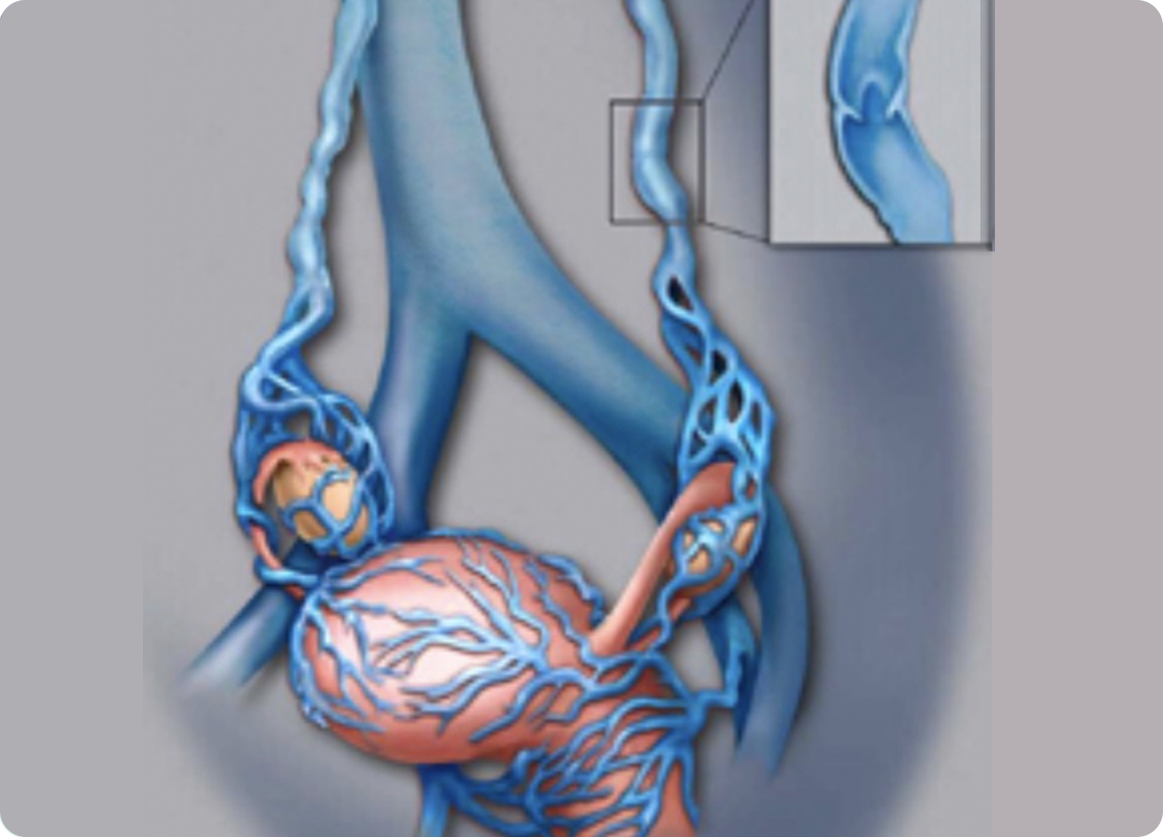
• Ovarian Vein Embolization: the abnormal ovarian vein is catheterized and then closed using a combination of coils (flexible platinum coils that block the vein) and sclerosent injection (a medication that shrinks and closes veins)

• Under sedation a catheter is placed via a vein either in the leg or just above the collarbone then directed into the ovary veins on each side
• Contrast (x-ray dye) is injected into each ovary vein, performing a venogram to tell if the vein is enlarged and malfunctions
• The abnormal ovary vein is then closed with a combination of coils and sclerosent.
• The procedure itself is successfully performed in nearly 100% of patients
• One of the largest and longest studies showed 83% of patients had significant improvement in symptoms

• The procedure is identical to ovarian vein embolization in women (see above)
• A catheter is positioned into each testicular vein and venogram performed to confirm the condition
• Abnormal testicular veins are closed using a combination of coils and sclerosent, administered through the catheter
• Success rates are 80-95%, equivalent to surgical treatment but with a much less invasive procedure and much shorter recovery.
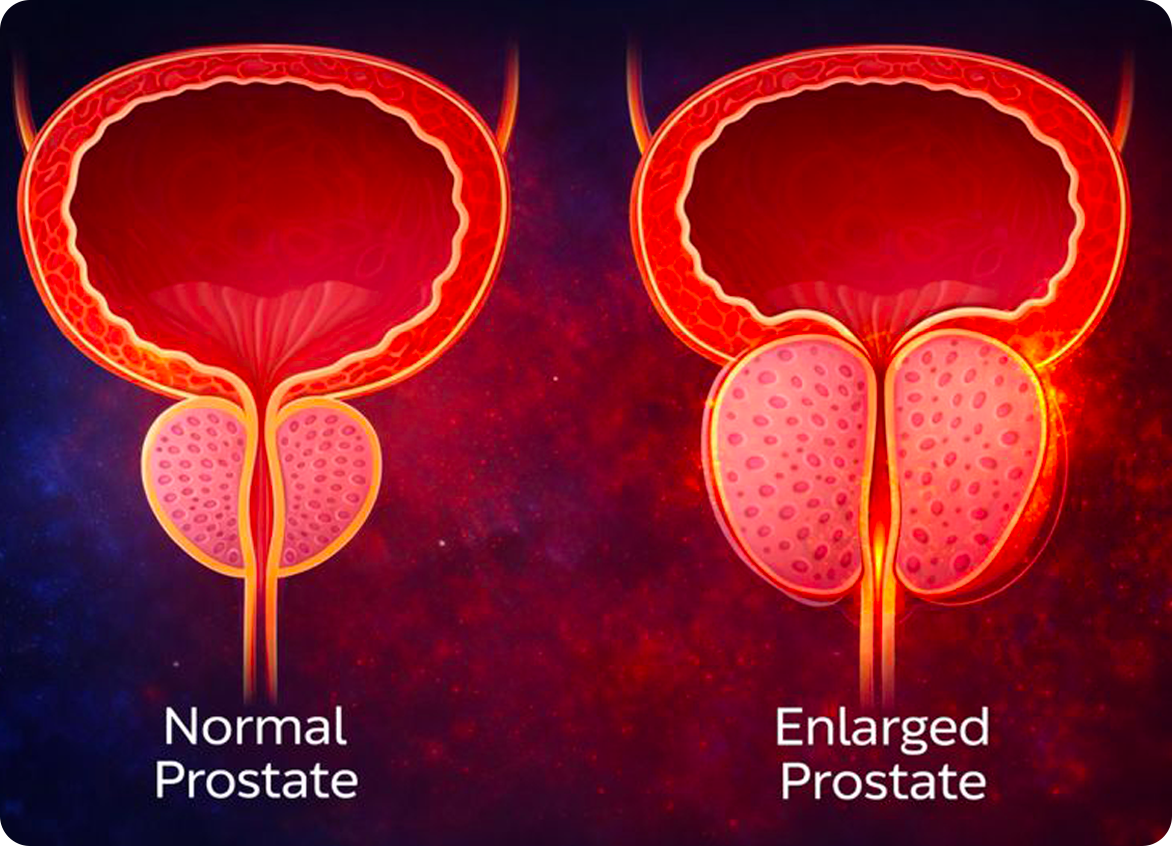
•Commonly known as an “enlarged prostate”
•Benign condition, but must be distinguished from prostate cancer by checking PSA level on a blood test and sometimes by performing an MRI
•BPH compresses the urethra just below the base of the bladder and reduced urine flow
•Symptoms include: frequent need to urinate, difficulty starting urination or completely emptying bladder, weak urine stream, and pelvic discomfort. A frequent symptoms is disruption of sleep due to need to get up and use bathroom multiple times throughout the night.
• Many patients are already aware of condition based on symptoms, previous prostate exam, or referral to a urologist
• A questionnaire helps measure the severity of symptoms
• Imaging such as ultrasound, CT, or MRI confirm the diagnosis and imaging exams are important to calculate the size of the enlarged prostate
• The first line of therapy is medications that can relax the prostate and bladder muscle to improve urine flow and also medications that can slowly reduce prostate size
• Transurethral Resection of the Prostate (TURP) was the gold standard for many years, involving removal of prostate tissue through a scope placed in the urethra
• Other less invasive surgical techniques include laser treatment and different ways of heating and shrinking the prostate through catheters inserted in the urethra
• Prostate Artery Embolization (PAE) is a relatively new procedure, first performed in the early 2000’s with many studies supporting its success performed from 2010 on.
• FDA approval was achieved in 2017, and the American Urological Association now supports PAE as a recommended, evidence-based treatment option as of 2023.

• A vascular procedure performed by an Interventional Radiologist, under sedation, a catheter is placed through an artery in the upper leg and positioned into the prostate arteries on each side, performing an angiogram to visualize the artery and guide treatment
• Small particles measuring a fraction of a millimeter are injected through a small catheter and into the prostate artery on each side, reducing blood supply to the prostate
• The reduction in blood flow causes the prostate to shrink over time, relieving pressure on the bladder and urethra and improving urine flow.
• A successful procedure is accomplished in 90% of patients
• 80-90% of patients treated with PAE have significant improvement in symptoms
• It is possible for the prostate to begin enlarging again in 5-10 years, but PAE can also be repeated, if necessary
If you are experiencing symptoms of PAD or are concerned about your vascular health,
[Request an Evaluation] to schedule an appointment. Early detection and treatment are key to managing PAD and
preventing further complications.